Why “no pain” doesn’t mean no damage — and what to do about it now
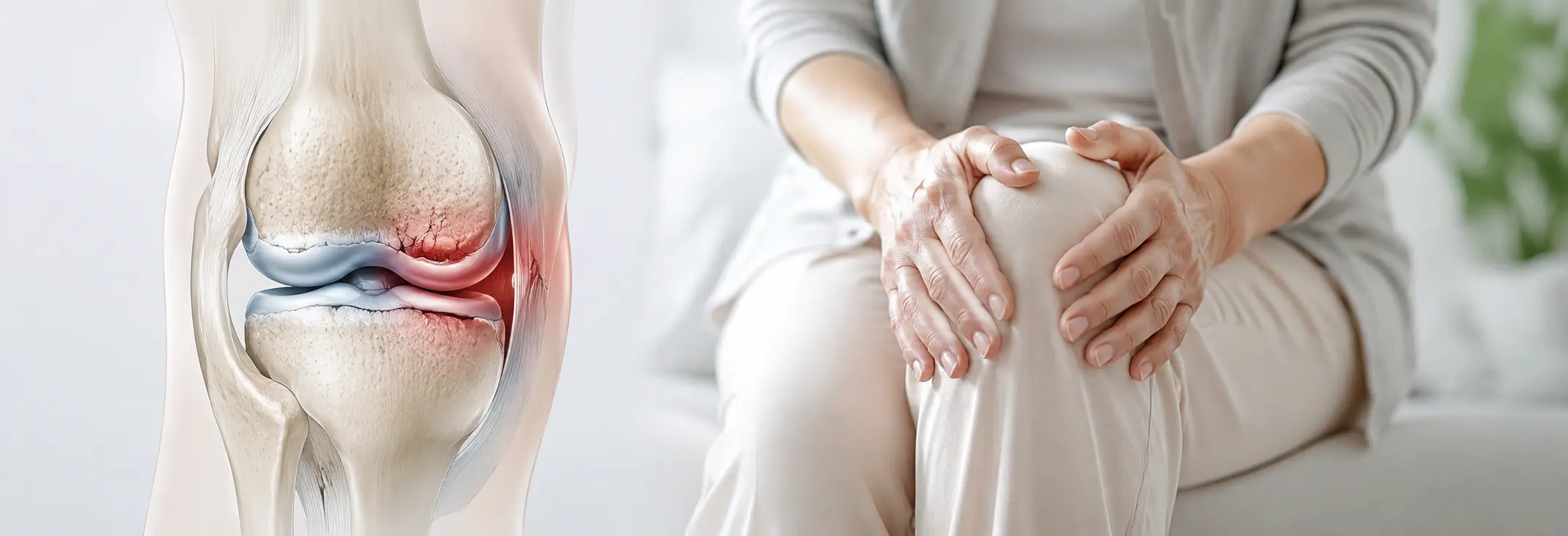
By the time osteoarthritis becomes painful, cartilage damage is often already significant. Because cartilage has almost no pain-sensing nerves, deterioration accumulates quietly, long before any symptoms appear. The most important window to protect your joints is right now — before the pain begins.
Note: The rate and pattern of joint deterioration varies between individuals. Not everyone will follow the same progression.
That first step out of bed feels heavier than it should. After hours at a desk, standing up comes with a familiar stiffness. Going downstairs, your knee gives way just a little. Most people meet these moments with a familiar reasoning: “It’s not really painful, I’ll keep an eye on it.” “It loosens up once I get moving.”
What often goes unnoticed is what’s happening inside the joint during that waiting period. A symptom disappearing is not the same as a joint recovering. The most important window to protect your joints is right now, before the pain begins.
Why Osteoarthritis Progresses Without Warning
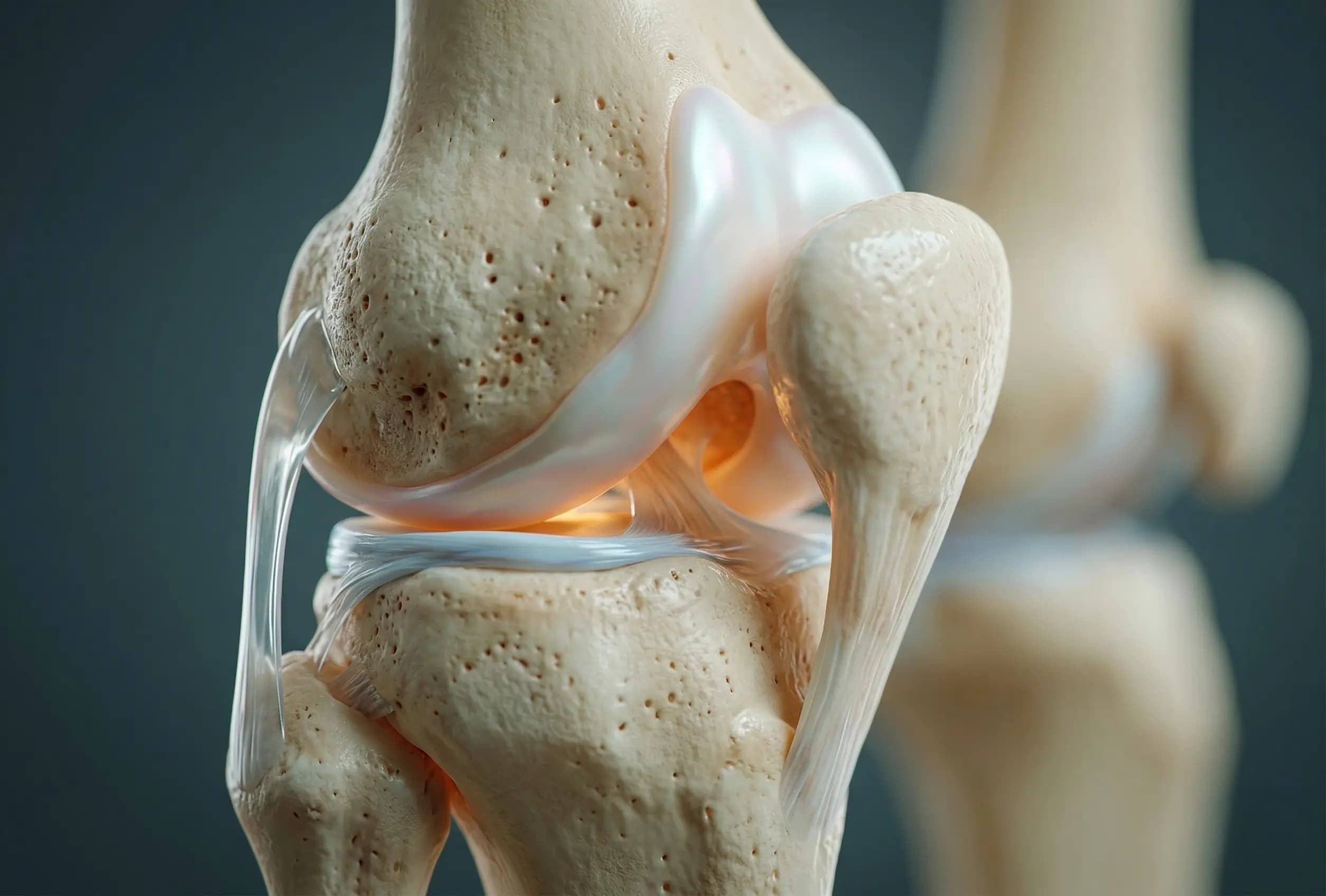
The most fundamental reason is that cartilage contains almost no pain-sensing nerves. Unlike muscle or skin, damaged cartilage sends no immediate distress signal to the brain. Deterioration accumulates quietly, entirely below the threshold of awareness.
Cartilage also has no direct blood supply. Once injured, it cannot draw on the nutrients that blood delivers, which makes natural repair extremely limited. The idea that careful use will allow cartilage to restore itself simply does not hold up.
As these factors compound, cartilage thins, synovial fluid diminishes, and bone-on-bone friction increases. Persistent pain typically does not appear until the joint has crossed into osteoarthritis. Pain is not the beginning of the problem — it is a delayed signal of a problem already well advanced.
When Should You Start? A Decade-by-Decade Guide
Some people sail through their thirties feeling fine, only to notice knee discomfort in their forties. Others manage their symptoms well into older age through consistent care. Knee health cannot be reduced to a matter of age alone. Worth noting: research shows that women develop osteoarthritis at roughly twice the rate of men (National Institutes of Health). The decline in estrogen following menopause is thought to reduce cartilage-protective function, making intentional knee care especially important for women in their fifties and beyond.
Is Your Knee Giving You Signals? A Quick Self-Check
Early signs are subtle and easy to dismiss. How many of the following sound familiar?
⚠ These symptoms may come and go. That cycle is not a sign of recovery — it may reflect shifting conditions inside the joint. Because cartilage has almost no pain-sensing nerves, deterioration can continue even during symptom-free periods. Dismissing these signs as trivial is one of the most common reasons minor damage becomes serious damage.
Seven Things You Can Do for Your Knees Starting Today
Protecting your joints is not about finding one perfect solution. It is about building several good habits and sticking with them.
When Lifestyle Changes Are Not Enough: Regenerative Medicine as an Option
Lifestyle modification is the foundation of joint care, and that will not change. But when it is no longer sufficient on its own, PRP therapy and adipose-derived stem cell (ASC) therapy may be worth considering. They become relevant in situations such as:
Note: PRP therapy and ASC therapy are performed in compliance with Japan’s Act on the Safety of Regenerative Medicine. Efficacy varies by individual. End-stage osteoarthritis (bone-on-bone) may fall outside the range where these treatments are applicable. We conduct a comprehensive assessment before recommending any treatment.
A Knee Health Checklist to Start Today
- ✓Strengthen the quadriceps, hamstrings, and hip abductors at least three times per week
- ✓Pay attention to movement mechanics when using stairs, rising from chairs, and lifting
- ✓Keep your weight within a healthy range to minimize ongoing joint load
- ✓Include anti-inflammatory foods in daily meals: fish, vegetables, and quality fats
- ✓Stay active within a pain-free range through walking, aquatic exercise, or similar activities
- ✓If any symptoms persist for more than two weeks, see a specialist rather than waiting
- ✓Confirm with a professional that past injuries have genuinely healed
“Pain is not the starting point. It is a signal that arrives late.” The earlier you act, the more you have to work with.
Note: This article is for general informational purposes only and does not guarantee specific treatment outcomes. ASC therapy is performed in compliance with Japan’s Act on the Safety of Regenerative Medicine, and results vary by individual.
Thinking About Next Steps?
If you have been wondering about the actual condition of your knee, here is a simple two-step starting point:
Step 1: Get an X-ray or MRI to establish a clear picture of your current joint health
Step 2: Bring your results to a regenerative medicine specialist to discuss whether conservative care is sufficient, or whether PRP or ASC therapy may be a relevant option for you
► Learn more about ASC therapy at Ginza YR ClinicConsultations & Appointments
References
- National Institute of Arthritis and Musculoskeletal and Skin Diseases. Osteoarthritis. https://www.niams.nih.gov/health-topics/osteoarthritis
- Loeser RF, et al. Osteoarthritis: A Disease of the Joint as an Organ. Arthritis Rheum. 2012.
- Katz JN, Arant KR, Loeser RF. Diagnosis and Treatment of Hip and Knee Osteoarthritis: A Review. JAMA. 2021.
- Chen D, et al. Osteoarthritis: Toward a Comprehensive Understanding of Pathological Mechanism. Bone Res. 2017.
- Pak J, et al. Adipose-derived stem cells and their secretome for knee osteoarthritis treatment. J Clin Med. 2018.